Spinal Conditions
 Low back pain is extremely common problem that most of us will experience at some point in their life time. About 8 in 10 people have one or more episodes of low back pain. In most cases, it is not due to a serious disease or serious back problem, and the exact cause of the pain is not clear. This is called nonspecific lower back pain. The usual advice is to keep active and do normal activities as much as possible. Painkillers can help until the pain eases. In most cases, the pain disappears within six weeks but may come back (recur) from time to time. Persistent (chronic) pain develops in some cases and further treatment may then be needed.
Low back pain is extremely common problem that most of us will experience at some point in their life time. About 8 in 10 people have one or more episodes of low back pain. In most cases, it is not due to a serious disease or serious back problem, and the exact cause of the pain is not clear. This is called nonspecific lower back pain. The usual advice is to keep active and do normal activities as much as possible. Painkillers can help until the pain eases. In most cases, the pain disappears within six weeks but may come back (recur) from time to time. Persistent (chronic) pain develops in some cases and further treatment may then be needed.
Low back pain symptoms range from sharp and stabbing to a dull ache. The pains can be constant or intermittent and positional. Acute low back pain can appear suddenly after injury.Most of low back pain resolves on its own and is often non-specific muscular origin from strain injury. A common cause of a sprain or strain is excessive physical demand on the spine’s ligaments or muscles due to combination of poor posture and prolonged sitting. Muscular back pain settles with course of physiotherapy concentrating on stretching and strengthening exercises for back muscles. Good posture care and ergonomics session will prevent recurrent episodes of muscular back ache.
Chronic low back often involves a disc problem, joint problem, or an irritated nerve root. Some ageing conditions that cause low back pain are Disc degeneration, Disc bulge, Disc Herniation (slipped disc), Sciatica, Spinal Stenosis (Spinal Canal Narrowing), Facet joint arthritis, Spondylolisthesis (Slipped Vertebra) and Sacroiliac Joint Dysfunction. If not treated on time, lower back pain can get severe affecting your daily living activities and quality of life.
Less common serious causes of back pain include infection (Spondylodiscitis), inflammation (Ankylosing Spondylitis, Rheumatoid arthritis), fracture, cauda equine syndrome and cancer (Primary/Metastasis) of the spine. There are symptoms and signs of back pain that indicate underlying serious spine condition. Knowing to spot those serious red flag symptoms will help early evaluation and treatment of the serious problem. Those red flag symptoms include constant and unrelenting back pain with any of following wide range symptoms and associated conditions
- Persistent fevers
- Unplanned weight loss
- Progressive numbness or weakness in the legs/feet
- Inability to urinate or have a bowel movement
- Loss of bowel/bladder control
- Pain at night
- Early morning pain and stiffness
- Sexual dysfunction
- Balance problems
- Pain not alleviated or worsened by different positions
- Recent IV drug use
- Progressive worsening of pain despite relative rest
- Recent trauma
- History of cancer
- History of diabetes mellitus
- History long term steroid medication
Some symptoms can come on suddenly while others can ramp up gradually. There are several conditions that can bring on these so-called red flags. Urgent spine specialist consultation is recommended if your back pain is of serious nature.
 Your neck is made up of vertebrae that extend from the skull to the upper torso. Cervical discs absorb shock between the bones.
Your neck is made up of vertebrae that extend from the skull to the upper torso. Cervical discs absorb shock between the bones.
The bones, ligaments, and muscles of your neck support your head and allow for motion. Any abnormalities, inflammation, or injury can cause neck pain or stiffness.
Many people experience neck pain or stiffness occasionally. In many cases, it’s due to poor posture or overuse. Sometimes, neck pain is caused by injury from a fall, contact sports, or whiplash.
Most of the time, neck pain isn’t a serious condition and can be relieved within a few days. This is usually because of muscular strain due to activities and behaviors such as poor neck posture, working at a desk for too long with flexed head posture, sleeping with your neck in a bad position and jerking your neck during exercise. Good physiotherapy and neck posture care sessions are all needed to resolve acute attack and minimize recurrent episodes of neck pain.
But in some cases, neck pain can indicate serious illness and require a spine specialist care. If you have neck pain that continues for more than a week, is severe, or is accompanied by other red flag symptoms, seek specialist attention immediately. Red flag symptoms are indicators of underlying serious spine illness such as disc bulge, spinal canal stenosis, infection, fracture, cancer, and rheumatoid arthritis and birth anomalies. Those red flag symptoms include constant neck pain, pain that radiates down your arms or legs, numbness or weakness of arms or legs, inability to move your arms or hands, inability to touch your chin to your chest, bladder or bowel dysfunction, and difficulty in balancing.
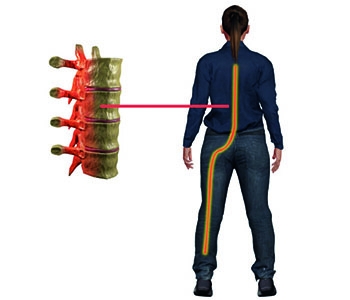 A disc bulge or herniation refers to a problem with one of the rubbery shock absorbing cushions (discs) that sit between the individual bones (vertebrae) that stack to make your spine.
A disc bulge or herniation refers to a problem with one of the rubbery shock absorbing cushions (discs) that sit between the individual bones (vertebrae) that stack to make your spine.
A spinal disc has a soft, jellylike center (nucleus) encased in a tougher, rubbery exterior (annulus). A bulging disc is a condition in which the nucleus (inner portion) of a spinal disc remains contained within the annulus fibrosus (outer portion), unlike a herniated disc in which the nucleus leaks out of the disc. Sometimes called a slipped disc or a ruptured disc, a herniated disk occurs when some of the nucleus pushes out through a tear in the annulus.
Most herniated disks occur in the lower back, although they can also occur in the neck. Signs and symptoms depend on where the disc is situated and whether the disc is pressing on a nerve. They usually affect one side of the body.
- Arm or leg pain.If your herniated disk is in your lower back, you’ll typically feel the most pain in your buttocks, thigh and calf. You might have pain in part of the foot, as well. If your herniated disk is in your neck, you’ll typically feel the most pain in your shoulder and arm. This pain might shoot into your arm or leg when you cough, sneeze or move into certain positions. Pain is often described as sharp or burning.
- Numbness or tingling.People who have a herniated disk often have radiating numbness or tingling in the body part served by the affected nerves.
- Muscles served by the affected nerves tend to weaken. This can cause you to stumble, or affect your ability to lift or hold items.
Natural history is that 70-80% of the disc herniation symptoms will resolve spontaneously in 6-12 weeks with non-operative treatment. Only those who have persistent symptoms beyond 2-3 months affecting their daily activities and quality of life will need disc removal surgery. Disc removal surgery (Discectomy) can be done as minimally invasive surgery with microscope or endoscope.
 Any degeneration of the vertebrae or disc, trauma, or fracture can cause spondylolisthesis. This occurs when one of the spinal bones (vertebra) slips forward onto the bone directly beneath it (falling out of alignment). Ageing related degenerative spondylolysthesis usually happens in the lower (lumbar) spine.
Any degeneration of the vertebrae or disc, trauma, or fracture can cause spondylolisthesis. This occurs when one of the spinal bones (vertebra) slips forward onto the bone directly beneath it (falling out of alignment). Ageing related degenerative spondylolysthesis usually happens in the lower (lumbar) spine.
Symptoms of Slipped Vertebrae can include persistent lower back pain, lower back tenderness, and radiating pain to thigh/leg, leg heaviness on standing/walking, stiffness in the back or legs, or numbness/weakness of legs/feet. Depending on the severity of the slip, symptoms intensity can vary from mild to severe affecting daily activities of life. Early spine specialist consultation for prompt diagnosis can be useful as delay can complicate the condition. First line of treatment includes simple analgesics, brace, exercises and physiotherapy. If non-operative treatment fails then surgery in the form of spinal fusion will provide long term pain/symptom relief to improve the quality of life.

Lumbar spinal stenosis is a narrowing of the spinal canal or open spaces in the spine, compressing the nerves travelling through the lower back (lumbar spine) into the legs. While it may affect younger patients, due to developmental causes or disc bulge, it is more often an ageing related degenerative condition that affects people who are typically age 60 and older.
Narrowing of the spinal canal usually occurs slowly, over many years or decades. The discs become less spongy with aging, resulting in loss of disk height, and may cause bulging of the hardened disk into the spinal canal. Bone spurs may also occur and ligaments may thicken. All of these can contribute to narrowing of the central canal and may or may not produce symptoms. Symptoms may be due to inflammation, compression of the nerve(s) or both.
Symptoms of spinal stenosis include:
Pain, heaviness, weakness or numbness in the legs, calves or buttocks
Pain worse with standing/walking and better with sitting/forward leaning or lying
Cramping in the calves with walking, requiring frequent short rests to walk a distance
Pain radiating into one or both thighs and legs (Sciatica type)
Weakness of legs, loss of normal bowel or bladder control
Symptoms can be severe enough affecting daily activities of living and quality of life. First line of treatment includes simple analgesics, brace, exercises and physiotherapy. If non-operative treatment fails then surgery will provide long term pain/symptom relief to improve the quality of life. There are different types of spinal surgeries available, and depending on the specific case, a spine surgeon will help to determine what procedure might be appropriate for the patient. The most common surgery in the lumbar spine is called decompressive laminectomy, in which the laminae (roof) of the vertebrae are removed to create more space for the nerves. Spine Surgeon may perform a laminectomy with or without fusing vertebrae or removing part of a disk. A spinal fusion with or without spinal instrumentation may be used to enhance fusion and support unstable areas of the spine. All these surgical interventions can be done through standard open approach or minimally invasive keyhole approach.
 Cervical discs are the cushions between the vertebrae in the upper back and neck. Herniation of the disc occurs when the gelatinous inner disc material, the nucleus pulpous, ruptures, or herniates, through the outer cervical disc wall.The causes may be due to ageing related degeneration of the disc, genetic problems, tobacoo use, poor neck posture, any sudden jarring movement, or any sudden stress that can damage the disk. Cervical disc herniation is usually seen in 30- to 50-year-olds
Cervical discs are the cushions between the vertebrae in the upper back and neck. Herniation of the disc occurs when the gelatinous inner disc material, the nucleus pulpous, ruptures, or herniates, through the outer cervical disc wall.The causes may be due to ageing related degeneration of the disc, genetic problems, tobacoo use, poor neck posture, any sudden jarring movement, or any sudden stress that can damage the disk. Cervical disc herniation is usually seen in 30- to 50-year-olds
Cervical disc herniation is a common cause of neck and upper body pain. Pain may feel dull or sharp in the neck, between the shoulder blades, and may radiate (travel) downward into the arms, hands and fingers. Sensations of numbness and tingling are typical symptoms, and some patients report muscle spasms. Certain positions and movement can aggravate and intensify pain. In some patients, a cervical herniated disc can cause spinal cord compression where disc material pushes on the spinal cord. This is a much more serious condition and may require a more prompt. Spinal cord compression symptoms include awkward or stumbling gait, difficulty with fine motor skills in the hands and arms, and tingling or “shock” type feelings down the torso or into the legs.
Natural history is that 70-80% of the disc herniation symptoms will resolve spontaneously in 6-12 weeks with non-operative treatment. Only those who have persistent symptoms beyond 2-3 months affecting their daily activities and quality of life will need disc removal surgery.
 Cervical myelopathy is a neck condition that arises when the spinal cord in the cervical spine region (neck) becomes compressed—or squeeze. Most common cause is the wear-and-tear (degenerative) changes that occur in the spine as we age. These degenerative changes in the discs are often called arthritis or spondylosis. The degenerative cervical myelopathy condition commonly occurs in patients over the age of 50. There are other non-age related conditions that can cause cervical myelopathy and they include rheumatoid arthritis infection (TB/bacterial), cancer, injury (traumatic disc herniation) and spinal cord abnormality/tumors.
Cervical myelopathy is a neck condition that arises when the spinal cord in the cervical spine region (neck) becomes compressed—or squeeze. Most common cause is the wear-and-tear (degenerative) changes that occur in the spine as we age. These degenerative changes in the discs are often called arthritis or spondylosis. The degenerative cervical myelopathy condition commonly occurs in patients over the age of 50. There are other non-age related conditions that can cause cervical myelopathy and they include rheumatoid arthritis infection (TB/bacterial), cancer, injury (traumatic disc herniation) and spinal cord abnormality/tumors.
Because the spinal cord carries nerve impulses to many regions in the body, patients with cervical myelopathy can experience a wide variety of symptoms. Weakness and numbness in the hands and arms, loss of balance and coordination, and neck pain/stiffness can all result when the normal flow of nerve impulses through the spinal cord is interrupted. Typical symptoms include gait imbalance or clumsiness of hands i.e. loss of fine motor skills with difficulty in handwriting, buttoning clothes, picking up coins, or feeding yourself. Severe spinal cord compression can cause paralysis and loss of bladder/bowel control (incontinence).
Cervical myelopathy is a progressive condition and can get worst over time. Non-operative treatment is the first line management for condition with static symptoms. Decompressive cervical spine surgery is recommended for worsening symptoms or cases presenting with severe spinal cord compression. Timely decompressive surgery before the development of paralysis or bladder/bowel incontinence is beneficial.
 Osteoporosis is a natural ageing phenomenon and a common condition that affects our bones as we age. Bone is living tissue that is constantly being broken down and replaced. Osteoporosis occurs when the creation of new bone doesn’t keep up with the loss of old bone. Osteoporosis develops slowly, and a person may not know they have it until they experience a fracture or break after a minor incident, such as a fall. Even a cough or sneeze can cause a break in osteoporotic bones. Osteoporosis causes bones to become weak and brittle — so brittle that a fall or even mild stresses such as bending over or coughing can cause a fracture. Osteoporosis-related fractures most commonly occur in the spine, hip, wrist, shoulder or ankle. A fracture is often a patient’s first sign of a weakened skeleton from osteoporosis.
Osteoporosis is a natural ageing phenomenon and a common condition that affects our bones as we age. Bone is living tissue that is constantly being broken down and replaced. Osteoporosis occurs when the creation of new bone doesn’t keep up with the loss of old bone. Osteoporosis develops slowly, and a person may not know they have it until they experience a fracture or break after a minor incident, such as a fall. Even a cough or sneeze can cause a break in osteoporotic bones. Osteoporosis causes bones to become weak and brittle — so brittle that a fall or even mild stresses such as bending over or coughing can cause a fracture. Osteoporosis-related fractures most commonly occur in the spine, hip, wrist, shoulder or ankle. A fracture is often a patient’s first sign of a weakened skeleton from osteoporosis.
Fractures caused by osteoporosis most often occur in the spine. These spinal fractures — called vertebral compression fractures are almost twice as common as other fractures typically linked to osteoporosis, such as broken hips and wrists. When the vertebrae bone in the spine weakens, they can narrow and become flatter. This can make elderly patients shorter and lead to a rounded back, a hump or a “bent forward look” to the spine (Senile Kyphosis). The weakened vertebrae are at a high risk for fracture. A vertebral compression fracture occurs when too much pressure is placed on a weakened vertebra and the front of it cracks and loses height. Vertebral compression fractures are often the result of a fall, but people with osteoporosis can suffer a fracture even when doing everyday things, such as reaching, twisting, coughing, and sneezing.
A vertebral compression fracture causes back pain. The pain typically occurs near the break itself. Vertebral compression fractures most commonly occur near the waistline, as well as slightly above it (mid-chest) or below it (lower back).
The pain often gets worse with movement, particularly when you are changing positions. It is often relieved by rest or lying down. Coughing and sneezing can also make the pain increase. Pain can be constant affecting daily activities of living.
First line of treatment is medical management with bone strengthening medication and brace support. Surgery is recommended when medical management fails and pain continues to affect quality of life. Surgery is minimally invasive keyhole procedure where the fractured vertebra bone is augmented with cement (Vertebroplasty/Kyphoplasty) and this is done as day care surgery. Cement augmentation surgery provides instant pain relief and return to normal day to day activities without pain.
 Spine is made up of 33 separate bones (vertebrae) plus many discs, ligaments and muscles which together form your spinal column. This surrounds and protects your spinal cord. A break, dislocation or ligament injury in any one of these bones can cause significant injury. Breaks can occur in the body of the vertebrae or to one of the processes or two vertebrae may detach (dislocate) from each other damaging surrounding ligaments. When any of these injuries occur it can also damage your spinal cord and might result in paralysis (loss of feeling and movement) below the level of the injury, reduced muscle power (weakness), altered sensations and muscle tone. This is because the messages in the brain can no longer travel down to the appropriate muscles as there is a break in the pathway.
Spine is made up of 33 separate bones (vertebrae) plus many discs, ligaments and muscles which together form your spinal column. This surrounds and protects your spinal cord. A break, dislocation or ligament injury in any one of these bones can cause significant injury. Breaks can occur in the body of the vertebrae or to one of the processes or two vertebrae may detach (dislocate) from each other damaging surrounding ligaments. When any of these injuries occur it can also damage your spinal cord and might result in paralysis (loss of feeling and movement) below the level of the injury, reduced muscle power (weakness), altered sensations and muscle tone. This is because the messages in the brain can no longer travel down to the appropriate muscles as there is a break in the pathway.
Road traffic accidents, falls and sports injuries are examples of trauma that can cause spine fractures and spinal cord injury. In an older person, the force needed to cause these injuries may be substantially less (thinning of the bones due to osteoporosis make them more fragile) causing the bones to break more easily.
Spine fractures caused by trauma can occur anywhere on the spine, including bones (vertebra) in the neck or cervical spine, bones in the upper back or thoracic spine, the lower back or lumbar spine, and the section of connected bone at the very bottom of the spinal column called the sacrum.
A spine fracture is a grave problem and this condition is serious and should not be neglected. A proper and timely intervention is highly advised.
Spinal fractures are managed differently depending on where they are located and what symptoms you are experiencing. Management may include surgery, a neck collar or a spinal brace, but some people do not require any of these. If you need to wear a collar or brace it may be required for up to twelve weeks after your injury. Surgery in the form of stabilization with or without decompression will be needed if stability of spinal column is in question.
Your rehabilitation from your injury will start as soon as you are able after management of your injury has been decided.

A spinal cord injury is damage to the spinal cord. It’s an extremely serious type of physical trauma that’s likely to have a lasting and significant impact on most aspects of daily life. The spinal cord is a bundle of nerves and other tissue that the vertebrae of the spine contains and protects. The vertebrae are the bones stacked on top of each other that make up the spine. The spine contains many nerves, and extends from the brain’s base down the back, ending close to the buttocks. The spinal cord is responsible for sending messages from the brain to all parts of the body. It also sends messages from the body to the brain. We’re able to perceive pain and move our limbs because of messages sent through the spinal cord.
If the spinal cord sustains an injury, some or all of these impulses may not be able to “get through.” The result is a complete or total loss of sensation and mobility below the injury. A spinal cord injury closer to the neck (cervical spine) will typically cause paralysis of all four limbs (quadriplegia) and injury in the mid or lower back (thoracic or lumbar spine) will cause paralysis of lower limbs (paraplegia)
Spinal cord injuries are generally caused by a direct trauma, for example a fall down stairs, sporting injury or road traffic accident, where a force to the spine causes the bone to break and impacts on the spinal cord. Other conditions that can cause spinal cord injury include cancer, osteoporosis, spine/spinal cord tumours, infection, inflammation of spine/spinal cord, spinal stenosis (narrowing of spinal canal space) and blood clot in spinal canal (haematoma).
Everybody with a spinal cord injury will experience slightly different symptoms, depending on the part of the spine that been injured and common symptoms include:
- Numbness below the level of the injury
- Significant muscle weakness below the level of the injury
- Changes in your bladder function being unable to urinate
- Changed in your bowel function being incontinent / or unable to initiate or control passage of stool
- Difficulty moving in bed
- Possible difficulty taking deep breaths or coughing
- Dizziness when sitting upright and reduced balance in sitting
- Difficulty with eating and drinking if your arms are paralysed
Spinal cord injury can be complete or incomplete. People with a complete spinal cord injury cannot move or feel anything at or below the area where the trauma occurred. Those with an incomplete spinal cord injury may have some sensation and movement below the level of the injury. Research suggests that people with an incomplete spinal cord injury have a higher chance of recovering from a loss of motor and sensory function in the affected limbs than those with a complete spinal cord injury.
Treatment and recovery time depend on the type of spinal cord injury that the person has sustained. Surgery is a standard treatment for spinal cord injuries. Surgery may involve the removal of objects compressing the spinal cord nerves, such as herniated disks, fractured vertebrae, or bone fragments.
Timely surgical intervention in the form of decompression (relieve pressure off spinal cord) and stabilisation of the spine will provide best chance for the recovery. After a spinal cord injury and initial surgical/medical management, you’ll need spinal cord injury rehabilitation to optimize recovery and adapt to a new way of life.
 A spinal infection is a rare, but often serious, form of disease that occurs when bacteria, fungi, or viruses invade the spinal tissues. These foreign agents can attack pretty much any part of the spine that you can image. This includes the vertebrae, spinal discs, spinal canal, meninges and even the spinal cord.
A spinal infection is a rare, but often serious, form of disease that occurs when bacteria, fungi, or viruses invade the spinal tissues. These foreign agents can attack pretty much any part of the spine that you can image. This includes the vertebrae, spinal discs, spinal canal, meninges and even the spinal cord.
Spinal infections may arise spontaneously or as a secondary condition, such as after an invasive medical procedure. Infections in the spine may affect different structures, such as the vertebral column bones (Osteomyelitis),intervertebral disc space (Discitis) and the spinal canal (Epidural Abscess). Certain factors increase your risk of developing spinal infections. Those risk factors include
- Malnourishment
- Immunosuppression caused by alcohol, chronic steroid use, autoimmune disorders or cancer
- Diabetes
- Haemodyalisis or renal failure
- Organ transplantation
- Drug addiction
- Recent urinary tract instrumentation
- Invasive spine surgery
- Elderly
Tuberculous infection of spine (Potts Disease) is very common, usually haematogenous (through blood stream) spread from lungs or other site of infection. 15% of patients with TB will present with spine infection.
Spine infection will present as constant back pain with associated symptoms of fever, chills, rigor, cough or unexplained weight loss. Back pain can be severe and may not relieve with rest or lying. Night pain is indicator of serious spine infection. If infection is severe then damage tof spinal nerves and spinal cord can present with numbness /weakness of limbs, bowel/bladder incontinence or paralysis.
Early diagnosis and timely management is all what needed for complete cure or clearance of the spine infection. Identification of the organism is essential, and this can be accomplished through keyhole surgery or computed tomography-guided biopsy sampling of the vertebra or disc space. Blood cultures, preferably taken during a fever spike, can also help identify the pathogen involved in the spinal infection. Proper identification of the pathogen (organism or bacteria) is necessary to narrow the antibiotic treatment regimen.
Spinal infections often require long-term intravenous organism specific antibiotic or antifungal therapy to clear the infection. Surgery in the form of abscess drainage, debridement, decompression and stabilisation will be required if there is instability of spine and patient presents with neurological deficit.
 Metastatic spinal tumors (cancer) are those that have spread to the spine from other areas of the body. If a tumor is able to spread, this usually means it is malignant. Between 30 and 70 percent of cancer patients develop metastatic spine cancer during the course of their disease. Lung, prostate, thyroid, kidney and breast cancers are the five most common cancers that tend to spread to the spine.
Metastatic spinal tumors (cancer) are those that have spread to the spine from other areas of the body. If a tumor is able to spread, this usually means it is malignant. Between 30 and 70 percent of cancer patients develop metastatic spine cancer during the course of their disease. Lung, prostate, thyroid, kidney and breast cancers are the five most common cancers that tend to spread to the spine.
Metastatic spine cancer present as back or neck pain depending on which part of spine is affected. Mid back (Thoracic) region is the most common site. Back pain is constant and may not relieve with painkillers or rest. Night pain is indicator of serious spine problem. If cancer destroys the spinal/vertebral column then spinal nerves/roots and spinal cord can be under pressure and present as neurological problems including radiating pain down arms/legs, numbness/weakness of arms/legs, bowel/bladder incontinence or paralysis.
Timely diagnosis and treatment is needed to relieve pain, improve neurological function and quality of life. Treatment strategy for spinal cancer and spinal tumors will differ based on the tumor type, aggressiveness and many other factors. Management can be palliative or curative and is best devised through multi-disciplinary team approach involving oncologist, pathologist, radiotherapist and surgeon. Spine surgery in form of surgical decompression and stabilisation of spine is recommended in patients presenting with neurological deficit and instability of spine. Post spine surgery radiotherapy and chemotherapy will be recommended depending on cancer type.

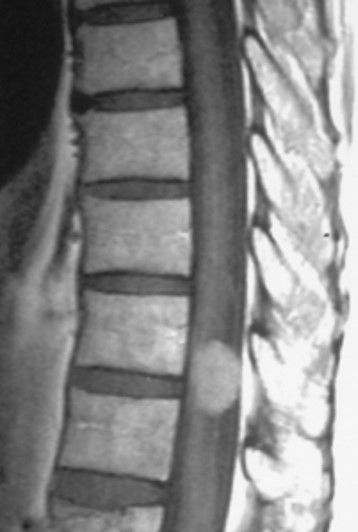 Primary spinal tumors are those that originate in the spine. They are relatively rare, typically benign (noncancerous) and represent a small percentage of spinal tumors. Malignant tumors (Osteosarcoma, Ewings, Chondrosarcoma) may also originate in the spine but are extremely rare.
Primary spinal tumors are those that originate in the spine. They are relatively rare, typically benign (noncancerous) and represent a small percentage of spinal tumors. Malignant tumors (Osteosarcoma, Ewings, Chondrosarcoma) may also originate in the spine but are extremely rare.
A primary spinal tumor is a serious issue and can cause pain, paralysis, or even neurological problems. Back pain is constant and may not relieve with painkillers or rest. Night pain is indicator of serious spine problem. If cancer destroys the spinal/vertebral column then spinal nerves/roots and spinal cord can be under pressure and present as neurological problems including radiating pain down arms/legs, numbness/weakness of arms/legs, bowel/bladder incontinence or paralysis.The condition if neglected can be even life-threatening too.
Timely diagnosis and treatment is needed to relieve pain, improve neurological function and quality of life. Treatment strategy for primary spinal tumous will differ based on the tumor type, aggressiveness and many other factors. Management is best devised through multi-disciplinary team approach involving oncologist, pathologist, radiotherapist and surgeon. Spine surgery can be palliative or curative and take form of excision of tumour, decompression/debulking, complete removal of tumor (enbloc, removal in toto), reconstruction and stabilisation. Pre or/ post spine surgery radiotherapy and chemotherapy will be recommended malignant spine cancer type.
 This is rare spinal condition (syndrome) that happens when the nerve roots of the cauda equina (collection of nerves at the end of the spinal cord) are compressed. It can disrupt the sensory and motor functions of the lower extremities and bladder. These nerves send and receive messages to and from the pelvic organs and lower limbs. It’s a medical emergency that needs urgent spinal surgical intervention.
This is rare spinal condition (syndrome) that happens when the nerve roots of the cauda equina (collection of nerves at the end of the spinal cord) are compressed. It can disrupt the sensory and motor functions of the lower extremities and bladder. These nerves send and receive messages to and from the pelvic organs and lower limbs. It’s a medical emergency that needs urgent spinal surgical intervention.
This usually occurs in adults, but sometimes can affect individuals of all ages and massive lumbar disc herniation compressing the cauda equine spinal nerve roots is the usual cause for it. Cauda equina syndrome can cause a variety of symptoms, including:
- Severe low back pain
- Bilateral or unilateral leg pain
- Bladder dysfunction such as urinary retention or incontinence (loss of control)
- Bowel incontinence (loss of control)
- Muscle weakness or sensory loss in both legs
- Loss of motor function in legs (difficulty walking)
- Loss or reduction of reflexes
- Saddle anesthesia (inability to feel anything in the body areas that would sit on a saddle)
Exact symptoms and their severity depend on which nerve root(s) are affected and the degree to which they are compressed.
This condition is a serious medical condition and can lead to permanent paralysis and bowel/bladder incontinence if not timely managed. Timely surgical intervention (with in 24-48 hrs of onset of urinary symptoms) in the form of decompression and disc removal surgery gives best chance for neurological recovery.
Paediatric Scoliosis Deformity:
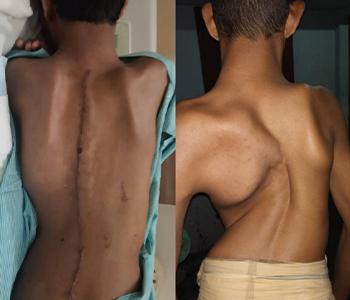 Scoliosis is an abnormal lateral curvature of the spine. It is most often diagnosed in childhood or early adolescence. The spine’s normal curves occur at the cervical, thoracic and lumbar regions in the so-called “sagittal” plane. These natural curves position the head over the pelvis and work as shock absorbers to distribute mechanical stress during movement. Scoliosis is often defined as abnormal spinal curvature (S or C shaped) in the “coronal” (frontal) plane. While the degree of curvature is measured on the coronal plane, scoliosis is actually a more complex, three-dimensional problem which involves coronal, sagittal and axial planes
Scoliosis is an abnormal lateral curvature of the spine. It is most often diagnosed in childhood or early adolescence. The spine’s normal curves occur at the cervical, thoracic and lumbar regions in the so-called “sagittal” plane. These natural curves position the head over the pelvis and work as shock absorbers to distribute mechanical stress during movement. Scoliosis is often defined as abnormal spinal curvature (S or C shaped) in the “coronal” (frontal) plane. While the degree of curvature is measured on the coronal plane, scoliosis is actually a more complex, three-dimensional problem which involves coronal, sagittal and axial planes
Scoliosis affects 2-3 percent of the population. Scoliosis can be present at birth or develop in infancy or early childhood or adolescence. Scoliosis is broadly classified as Early Onset Scoliosis when scoliosis is present at birth or diagnosed before the age of 10 year or Late Onset Scoliosis when scoliosis develops after the age of 10 years (10-15 years). Scoliosis in children is also classified by age: 1.) Infantile (0 to 3 years); 2.) Juvenile (3 to 10 years); and 3.) Adolescent (age 11 and older, or from onset of puberty until skeletal maturity).
Scoliosis can be classified by etiology (cause): idiopathic (unkown cause), congenital (birth anomalies) or neuromuscular (nervous/muscle problem). Idiopathic scoliosis is the diagnosis when all other causes are excluded and comprises about 80 percent of all cases. Adolescent idiopathic scoliosis is the most common type of scoliosis and is usually diagnosed during puberty.
Congenital scoliosis results from embryological malformation of one or more vertebrae and may occur in any location of the spine. The vertebral abnormalities cause curvature and other deformities of the spine because one area of the spinal column lengthens at a slower rate than the rest. The geometry and location of the abnormalities determine the rate at which the scoliosis progresses in magnitude as the child grows. Because these abnormalities are present at birth, congenital scoliosis is usually detected at a younger age than idiopathic scoliosis.
Neuromuscular scoliosis encompasses scoliosis that is secondary to neurological or muscular diseases. This includes scoliosis associated with cerebral palsy, spinal cord trauma, muscular dystrophy, spinal muscular atrophy and spina bifida. This type of scoliosis generally progresses more rapidly than idiopathic scoliosis and often requires surgical treatment.
Early onset scoliosis can be congenital or neuromuscular or idiopathic variant and tend to affect boys more than girls. Late onset scoliosis is mostly Adolescent Idiopathic Scoliosis variant and tend to affects more girls than boys. There are several signs that may indicate the possibility of scoliosis. If one or more of the following signs is noticed, consult spine specialist.
- Shoulders are uneven – one or both shoulder blades may stick out
- Head is not centered directly above the pelvis
- One or both hips are raised or unusually high
- Rib cages are at different heights
- Rib hump where ribs stick out unevenly
- Waist is uneven
- The appearance or texture of the skin overlying the spine changes (dimples, hairy patches, color abnormalities)
- The entire body leans to one side
Scoliosis is usually confirmed through a physical examination and static and dynamic radiographs (X-rays). CT scan or MRI is done to assess bony or spinal cord abnormality as part of management plan. The curve is measured by the Cobb Method and is diagnosed in terms of severity by the number of degrees. A positive diagnosis of scoliosis is made based on a coronal curvature measured on a posterior-anterior radiograph of greater than 10 degrees. In general, a curve is considered significant if it is greater than 25 degrees. Curves exceeding 45 to 50 degrees are considered severe and often require more aggressive treatment.
A standard exam that is sometimes used by doctors and nurse is called the Adam’s Forward Bend Test. During this test, the patient leans forward with his or her feet together and bends 90 degrees at the waist. From this angle, any asymmetry of the trunk or any abnormal spinal curvatures can easily be detected by the examiner. This is a simple initial screening test that can detect potential problems, but cannot determine accurately the exact type or severity of the deformity. Radiographic tests are required for an accurate and positive diagnosis.
When there is a confirmed diagnosis of scoliosis, there are several issues to assess that can help determine treatment options:
- Spinal maturity – is the patient’s spine still growing and changing?
- Degree and extent of curvature – how severe is the curve and how does it affect the patient’s lifestyle?
- Location of curve – according to some experts, thoracic curves are more likely to progress than curves in other regions of the spine.
- Possibility of curve progression – patients who have large curves prior to their adolescent growth spurts are more likely to experience curve progression.
After these variables are assessed, treatment options recommended are observation, bracing or surgery.
Observation:
In many children with scoliosis, the spinal curve is mild enough to not require treatment. However, if there is concern that curve would progress with time, then close monitoring of the child every four to six months throughout adolescence is considered..
Bracing:
Braces are only effective in patients who have not reached skeletal maturity. If the child is still growing and his or her curve is between 25 degrees and 40 degrees, a brace may be recommended to prevent the curve from progressing. There have been improvements in brace design and the newer models fit under the arm, not around the neck. There are several different types of braces available. While there is some disagreement among experts as to which type of brace is most effective, large studies indicate that braces, when used with full compliance, successfully stop curve progression in about 75% percent of children with scoliosis. For optimal effectiveness, the brace should be checked regularly to assure a proper fit and may need to be worn 16 to 23 hours every day until growth stops.
Surgery:
In children, the two primary goals of surgery are to stop the curve from progressing during adulthood and to correct spinal deformity. Most experts would recommend surgery only when the spinal curve is greater than 40 degrees and there are signs of progression. This surgery can be done using an anterior approach (through the front) or a posterior approach (through the back) depending on the particular case.
Posterior Scoliosis Correction and Fusion: The most frequently performed surgery for adolescent idiopathic scoliosis involves traditional posterior spinal fusion with instrumentation and bone grafting. This is performed through the back while the patient lies on his or her stomach. During this surgery, the spine is straightened with rigid rods, followed by spinal fusion. Spinal fusion involves adding a bone graft to the curved area of the spine, which creates a solid union between two or more vertebrae. The metal rods attached to the spine ensure that the backbone remains straight while the spinal fusion takes effect. This procedure usually takes several hours in children. With recent advances in technology, most people with idiopathic scoliosis are released from hospital within a week of surgery and do not require post-surgical bracing. Most patients are able to return to school or work in two to four weeks post surgery and are able to resume all pre-surgical activities within four to six months.
Anterior Scoliosis correction and Fusion: The patient lies on his or her side during the surgery. The surgeon makes incisions in the patient’s side, deflates the lung and removes a rib in order to reach the spine. Video-assisted thoracoscopic (VAT) surgery offers enhanced visualization of the spine and is a less invasive surgery than an open procedure. The anterior spinal approach has several potential advantages: better deformity correction, quicker patient rehabilitation, improved spine mobilization and fusion of fewer segments. The potential disadvantages are that many patients require bracing for several months post surgery, and this approach has a higher risk of morbidity – although VAT has helped to reduce the latter.
Non Fusion/Dynamic Anterior Scoliosis Correction Surgery (Anterior Vertebral Body Tethering): Over the past 100 years, significant advancements have been made in spinal fusion to treat scoliosis. These advancements have led to improved fusion rates, lower complication frequency, greater three-dimensional correction of the deformity and more rapid postoperative recovery. However, spine fusions mean fewer motion segments (less spine motion), which may lead to lower function in high-level physical activity (e.g. competitive athletics) and greater chance for spine arthritis. As a result, preservation of spinal motion, particularly in the low back, is an important goal.
The desire to maintain spine motion has fueled the development of various growth modulation procedures. The goals of these procedures are to correct the spinal deformity and maintain motion/flexibility (without fusion). One of these promising techniques that have gained traction in the last 10 years is vertebral body tethering (VBT). This technique uses the growth modulation principles where it places a compressive force over the convex side of the spine (slowing down growth) to permit the concave side of the spine to relatively grow more and create a straighter spine through remaining growth potential of the child. There is significant potential for this technology and early clinical results are promising but the technology is still under scrutiny and close monitoring.
In children with Early Onset or Congenital scoliosis, there is a known increased incidence of other congenital abnormalities. These are most commonly associated with the spinal cord (20 percent), the genitourinary system (20 to 33 percent) and the heart (10 to 15 percent). It is important that evaluation of the neurological, genitourinary and cardiovascular systems is undertaken when congenital scoliosis is diagnosed. Management of Early onset or congenital scoliosis is challenging and treatment has to commence at very early age to control the curve and allow spinal growth thereby allowing lung development and maturity. Casting, bracing and temporary growth rod distraction techniques are used with closed monitoring until the child attains reasonable skeletal maturity at which point definitive spinal fusion and scoliosis correction is considered.
Paediatric Kyphosis Deformity:
Kyphosis is a spinal disorder in which an excessive outward curve of the spine results in an abnormal rounding of the back. The condition is sometimes known as “roundback” or in the case of a severe curve as “hunchback.” Kyphosis can occur at any age, but is common during adolescence.
Kyphosis is children can be due to Scheuermann’s disease, vertebral anomalies (birth defect) or infection (Tubercolosis, Kochs/Potts spine).
One particular type of kyphosis is Scheuermann’s kyphosis, also known as Scheuermann’s disease. Scheuermann’s kyphosis is characterized by wedge-shaped vertebrae that cause the thoracic spine to curve forward too much. Scheuermann’s kyphosis develops over time during periods of bone growth (such as puberty). It occurs when the front of the spine doesn’t grow as fast as the back of the spine and causes healthy, rectangular-shaped vertebrae to become triangular-shaped and wedged together. This causes the thoracic spine to curve more than normal. Patients become stooped forward with a bent-over posture. The exact causes of Scheuermann’s kyphosis are still unknown; however, researchers believe it has something to do with interrupted bone growth or an abnormality in how vertebrae develop and grow. This condition seems to run in families. Height and weight may also be contributing factors.
Kyphosis will present a spoor posture or slouching, rigid deformity, fatigue and back pain, neurological symptoms, and breathing difficulty because of impaired lung function in severe deformity.
Treatment options are observation, bracing or surgery
Observation and bracing are recommended if the curve or deformity is milder (40-70 degrees) and child has no associated pain or neurological symptoms.
Surgery is recommended when the deformity is severe (curve >70 degrees) or presenting neurological symptoms. Posterior correction and instrumented fusion is the standard surgical intervention.
 Scoliosis (sideways curvature) or Kyphosis (round/hunch back) that occurs or is diagnosed in adult is distinctive from childhood scoliosis, since the underlying causes and goals of treatment differ in patients who have already reached skeletal maturity.
Scoliosis (sideways curvature) or Kyphosis (round/hunch back) that occurs or is diagnosed in adult is distinctive from childhood scoliosis, since the underlying causes and goals of treatment differ in patients who have already reached skeletal maturity.
Most adults with scoliosis can be divided into the following categories: 1.) Adult scoliosis patients who were surgically treated as adolescents; 2.) Adults who did not receive treatment when they were younger; and 3.) Adults with a type of scoliosis called degenerative scoliosis.
Degenerative scoliosis occurs most frequently in the lumbar spine (lower back) and more commonly affects people age 65 and older. It is often accompanied by spinal stenosis, or narrowing of the spinal canal, which pinches the spinal nerves and makes it difficult for them to function normally. Back pain associated with degenerative scoliosis usually begins gradually and is linked with activity. The curvature of the spine in this form of scoliosis is often relatively minor, so surgery may only be advised when conservative methods fail to alleviate pain associated with the condition.
Some adults who previously had single or multi level fusion surgery may develop problems at the adjacent level either at the top or bottom of the previously fused segments as the remaining mobile segments assume much more of the load and the stress associated with movements. Adjacent segment disease is the process in which degenerative changes occur over time in the mobile segments above and below the spinal fusion. This can result in painful arthritis of the discs, facet joints and ligaments.
Age-related Kyphosis is common and is often due to weakness in the spinal bones (osteoporosis) that causes them to compress or crack.
In general, surgery in adults with degenerative scoliosis or kyhosis may be recommended when the spinal curvature presents with sever back pain, leg pain and neurological symptoms affecting her daily living activities. Adults with degenerative scoliosis and sagittal imbalance will mostly present with back pain and /or spinal stenosis (claudication) may require decompression surgery with spinal fusion. Surgical intervention for adult spinal deformity in elderly patients is quality of life improvement procedure,